 Anesthesia and Diabetes Mellitus
Anesthesia and Diabetes Mellitus
Clinical Manifestations of Diabetes Mellitus (DM)
Insulin deficiency leads to hyperglycemia and glycosuria.
-
Fasting blood glucose > 126 mg%
GTT: blood glucose > 200 mg%
-
Type I Immune-mediated or idiopathic absolute insulin deficiency
-
onset < 16 years old
15% have other autoimmune disease
-
hypothyroidism
Graves' disease
Addison's disease
myasthenia gravis
Type III Secondary to specific genetic defects
Type IV Gestational
-
2.4% of U.S. pregnancies
-
Hypertension
- risk of MI 2-10 X greater than in nondiabetic
- risk of peripheral vascular disease 5-10 X greater than in nondiabetic
- risk of stroke twice that in nondiabetic
- >15% of diabetics
- increases perioperative morbidity
Myocardial infarction
- Diabetic ketoacidosis (DKA)
usually Type I - Hyperosmolar nonketotic coma
- Hypoglycemia
-
Dyspnea, abdominal pain, nausea and vomiting, dehydration, coma
Anion-gap metabolic acidosis, elevated plasma and urine ketones (acetoacetate, beta-hyroxybutyrate), hyperglycemia
Rx
-
Insulin (regular) 0.1 U/kg/hour and increase
NS
Potassium when urine output
Add D5W when plasma glucose 250 mg%
-
Hyperglycemic diuresis -> severe dehydration
Renal failure
Lactic acidosis
Risk of intravascular thromboses
Hyperosmolality with coma � seizures
Rx
-
Fluid resuscitation
Insulin (relatively small doses)
Potassium when urine output
-
Diaphoresis, tachycardia, nervousness
Plasma glucose < 50 mg%
Rx: D50W
Anesthetic Considerations
Preoperative-
Evaluate end-organ damage (cardiovascular, pulmonary, renal)
- 30-40% of Type I diabetics
- positive "prayer sign" (image at right:)
- TJ joint and C-spine (e.g. atlanto-occipital joint) may be involved
- good measure of overall blood glucose control
- normal 5-7%
- up to 20% in marked hypergylcemia
Beware silent myocardial ischemia/infarction
Diabetic autonomic neuropathy
-
Hypertension
Painless myocardial ischemia
Orthostatic hypotension
Lack of heart rate variability
Reduced heart rate response to atropine or propranolol
Resting tachycardia
Early satiety
Neurogenic, atonic bladder
Lack of sweating
Impotence
Asymptomatic hypoglygemia
Sudden death syndrome
Mortality 50% over 5 years
-
Consider H-2 blocker or metoclopramide premed
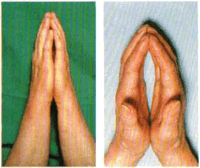
Direct laryngoscopy may be difficult in 30% of Type I diabetics
Glycohemoglobin, hemoglobin A1c
-
Insulin/glucose regimens (after starting IV and checking blood glucose)
- 1/2 of total daily dose as intermediate form (NPH) + intraop "sliding scale," or
- Continuous infusion of regular insulin
-
U/hr = (plasma glucose)/150 +
-
Start IV and check blood glucose
Begin D5W 1 - 1.5 ml/kg/hr (IV 'piggy-back')
Administer insulin: either
Avoid hypoglycemia
Hyperglycemia:
-
Hyperosmolarity
Infection
Poor wound healing
Worsens neurologic outcome after cerebral ischemia
-
Monitor blood glucose